Patients who need a new liver to survive must hope that they are one of the approximately 13,000 liver transplant recipients in the United States and Europe each year. But with 30,000 people on waiting lists, and with only ice keeping livers for transplantation viable for up to 14 hours, the odds are not always in the patients’ favor. Each year, more than 2,000 livers don’t survive the journey to their new home.
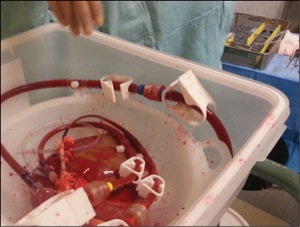 A liver 30 seconds after connection to the OrganOx Metra device. Parts of the organ are still cold, while other parts are warm and perfused with red cell solution. |
“Preserving organs by cooling them down is far from perfect,” said Peter J. Friend, MD, director of transplantation surgery, Nuffield Department of Surgical Sciences, Oxford Transplant Centre, U.K. “Although cooling the organ on ice slows its metabolism by a factor of 10, the liver continues to metabolize slowly and deteriorates as a result. It’s hard to tell which organs will work and which ones won’t.”
Now, however, Dr. Friend and his colleague Constantin Coussios, PhD, professor of biomedical engineering at the University of Oxford, have devised a novel technology that may be a game changer: A machine that allows the liver to function for up to 24 hours, as though it were still inside a human body.
On March 15, the team of engineers and physicians announced the preliminary success of this machine, which has safely transported livers to two transplant recipients at King’s College Hospital in London.
“The first two cases went very well,” said Dr. Friend. “They weren’t exceptionally high risk, but the machine did what it was supposed to do.”
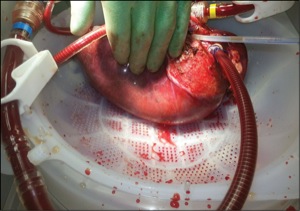 The liver 5 minutes after connection to the OrganOx Metra, now fully perfused and at physiologic temperature. |
Long Time in the Making
In 1994, Drs. Friend and Coussios devised the idea for the technology, but faced several engineering challenges while developing it. The co-inventors needed to create an artificial environment, that could simulate the key functions of the human body, including pumping blood and providing nutrition to the organ. These functions not only had to be automated to make it possible for transplant surgeons around the globe to use the technology, but also small enough for easy transportability.
After 15 years of developing and tweaking the design, Drs. Friend and Coussios have created a technology that appears to meet these requirements. The liver’s main blood vessels are connected to tubes on the machine, which automatically regulate the environment around the liver. The device maintains the liver at body temperature and infuses it with oxygenated red blood cells, nutrition such as glucose and amino acids, and other chemicals to create a physiologic environment that mimics the human body. The liver is not only kept alive, but it continues to produce bile as well.
Additionally, the machine is compact.
“It’s about the size of a supermarket trolley [shopping cart], which means it can go in back of ambulance, small plane or helicopter,” Dr. Friend said. “Size was very important because we knew there was no point in making a machine if it couldn’t fit in the back of a vehicle.”
Notably, the machine also may allow the liver to recover from injuries it sustained during or before removal, Dr. Friend pointed out. This function of the device is particularly important because it could expand the number of viable livers for transplantation. In recent years, the demand for livers has grown, as liver disease has become more common, whereas the quality of donor livers has diminished.
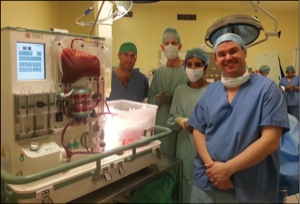 The King’s College Hospital, Oxford University and OrganOx team successfully connects the first human liver for transplantation to the OrganOx Metra device. |
“More and more, donors tend to be older, and have a high body mass index or coexisting major health problems,” Dr. Friend noted. “Because of the increasing demand for livers, we are having to use organs we would have once said no to.”
Now with the machine, transplant surgeons can test how well the liver is working during preservation.
“If the liver works on the pump, then we can assume it will work in the recipient,” said Maria B. Majella Doyle, MD, MBA, associate professor of surgery at Washington University School of Medicine, St. Louis, who specializes in liver transplantation. Dr. Doyle was not involved in developing this pump, but she is performing research to develop a different liver pump system, one that also keeps the liver at physiologic temperature.
In April 2008, Drs. Friend and Coussios cofounded a company called OrganOx Ltd., to continue their University of Oxford research. With financial support from the Royal Society and several venture capital funds in the United Kingdom, the company has been working to bring the technology to patients.
Although promising, the device still needs more testing. The U.K. team has begun a pilot trial at King’s College Hospital to test the ability of the machine to transport livers to 20 transplant patients. If the trial is successful, OrganOx then could apply for marketing authority, which would make the device commercially available in Europe.
“If the machine is as good as we believe, we would expect a significant increase in patients who get liver transplants,” Dr. Friend said.
According to Dr. Doyle, the group is “ahead of the game.” To her knowledge, two other teams are developing physiologic-temperature liver pump systems—Dr. Doyle and her colleagues William Chapman, MD, and Vijay Subramanian, MD, at Washington University, and Constantino Fondevila, MD, PhD, at the University of Barcelona—but both are at more preliminary stages.
“The U.K. team is the first to produce human data with the pump and show it’s safe and viable as a liver transplantation device. Now, it’s important to make sure the technology is foolproof and cost-effective,” Dr. Doyle said.
“The U.K. team needs to be highly commended. The pump is a great achievement.”
“You Have the Power to Donate Life – Sign-up today! Tell Your Loved Ones of Your Decision”
2 comments:
This is a great idea. I hope it pushes through. A lot of awaiting patients have missed the opportunity of receiving organs because it's either they come from too far away places or damaged ones already. Now, if this device will help keep these organs alive with the use of this device, then it think it ought to be given a chance.
- AcuteAir.com
This is interesting and brilliant. If this project will come through,it is going to benefit a lot of patients. Keeping organs outside the body have been a problem and if this will help solve that problem, then by all means.
- AcuteAir.com
Post a Comment